A Machine With Real Heart

In September 1958, Helen Harris was ten years old with a congenital heart defect. “I was the first in New Zealand to have hole-in-the-heart surgery with the heart-lung machine - a great step forward for medical science.” Her operation took place at Green Lane Hospital in Auckland, using the Melrose heart-lung machine which is now in MOTAT’s collection.
Denis Melrose developed the heart-lung machine while working at the Royal Postgraduate Hospital Hammersmith in the United Kingdom where it was first used for successful open-heart surgery in 1957. The machine was built by the medical instrument firm, NEP (New Electronic Products) owned by Francis Kellerman.

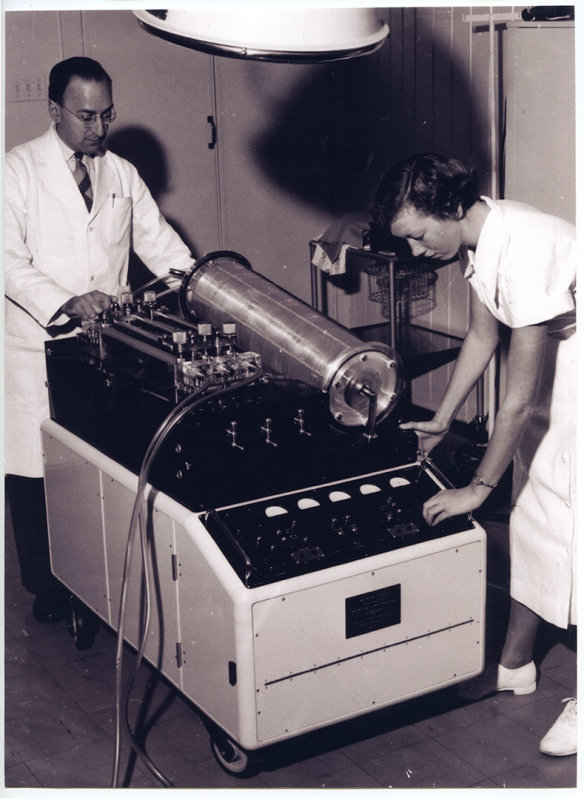
A heart-lung machine works on a simple principle in a continuous loop. Blue blood is drawn from the heart and drained into a reservoir from which it is pumped into an artificial lung or oxygenator – in the Melrose heart-lung machine this is discs of Perspex which can be seen in the photo above (the clear circular drum on the right). As the blood trickles down through the discs, oxygen gas is delivered to it which allows the blood cells to absorb oxygen molecules directly. The blood turns red during this process. The heart-lung machine then pumps the red blood back into the patient.
Brian Barratt-Boyes who had been recruited as a senior cardio-thoracic surgeon in 1957 by Sir Douglas Robb, the surgeon-in-charge at Auckland’s Green Lane Hospital, recommended that the hospital purchase a Melrose heart-lung machine so that the cardiac team could perform open-heart surgery.
Sid Yarrow, a Green Lane Hospital laboratory technician at the time, recalled that when the Melrose arrived in Auckland in 1957, it came in a huge wooden box. He opened the box “And there it was. There was no literature with it, nothing.” He was somewhat taken aback and wrote to the manufacturer asking for more information. “They did actually send me a circuit diagram of the electronic controls, so I was able to follow that and work on it.” He remembered that he and Brian Barratt-Boyes looked at all the parts and realised that “There were many parts which were totally inexplicable to us, and we discarded them. B-B said, ‘It won’t work the way it is. We need to develop it further.’ So, he had ideas, and I had ideas, and we pooled our ideas worked on it for the best part of a year.’
Sid explained that “There was no mechanism for controlling the flow of oxygen and I had to incorporate a gas flow meter into that. The oxygenator consisted of hundreds of discs of Perspex. Perspex melts at high temperatures, and so you can’t sterilise it by heat. And there were no indications of how to sterilise it.” Sid had heard about a new form of sterilising using ethylene oxide gas which was very effective and dissipated quite quickly. He found a steriliser in the Auckland Hospital Board’s salvage store and had it delivered to Greenlane.
“We arranged for our hospital engineers to provide a heating system to warm it,” Sid added. “We also needed to have a pump to suck out the air, and then a container to admit the [oxygen] gas which came in canisters. We used a milking machine pump, which worked very nicely, a vacuum pump.”
“We had heard that a hospital in Sydney was using ethylene oxide and so I wrote to a contact there and begged a few cans of that gas, and they lent us some…which were pretty precious to us. And we built this steriliser. It worked very well after some modifications. That was the first time ethylene oxide had ever been used in this country. It’s now widely used in every hospital,” he concluded.
In 1958 the heart team began to practise open heart surgery on animals. Brian Barratt-Boyes and his team began with small animals and then moved to sheep which have a heart similar in size to a human’s. They performed surgery on one sheep a week for 17 weeks without any deaths and then Barratt-Boyes decided it was time to make the move to human hearts.
Helen Harris was a ‘blue baby’, born with a congenital heart defect. She was the first human in New Zealand to have open-heart surgery using the Melrose heart-lung machine, and she takes up the story: “I was the first in New Zealand to have hole-in-the-heart surgery with the heart-lung machine - a great step forward for medical science, “ she said. “I was called to Green Lane Hospital in June [1958] for tests and was made a candidate for open heart surgery later that year. I returned on the 23rd of August. There were six children of all ages from around the country to have this operation. All our parents were interviewed, and, out of that, my mother and father were chosen to give permission for this operation. The date set: 3 September 1958.”
Helen continued, “The day dawned. I clearly remember missing my breakfast that morning. The preparations began and I was wheeled down to the theatre in my bed and put to sleep. My next memory is waking up in an oxygen tent in a room full of strange noises generated by machines all about the room.”
Helen was only ten years old and “Was unaware of the importance of the occasion and how relieved the wonderful medical team and my parents must have been.” Indeed.
Helen recalls that she was not told how revolutionary her operation would be. “Mum and Dad, I don't think, really knew. They hoped. On the day, Mum and Dad went out and walked up One Tree Hill and prayed and spent their day doing exactly that,” she said.

The combination of Denis Melrose’s invention, Brian Barratt-Boyes's determination, and Sid Yarrow’s ingenuity – along with input from others at Green Lane Hospital – saved Helen Arnold’s life and gave her a long and fruitful life.

Story by Megan Hutching, Oral Historian, MOTAT
Links:
Heart and Lung Machine [Melrose]
MOTAT Collection Item
Melrose, Denis Graham (1921 - 2007)
Citation:
Hutching, Megan. 2021. The Melrose heart and lung machine. New Zealand: The Museum of Transport and Technology (MOTAT). First published: 16 November 2021. URL www.motat.nz/the-melrose-heart-lung-machine